Abcuro is advancing first-in-class programs in autoimmunity and cancer in which highly cytotoxic immune cells play a critical role.

Ulviprubart is a first-in-class anti-KLRG1 antibody capable of selectively depleting highly cytotoxic T cells, while sparing naïve, regulatory and central memory T cells. Ulviprubart has been designed to treat diseases mediated by highly cytotoxic T cells, including the autoimmune muscle disease inclusion body myositis (IBM), T cell large granular lymphocytic leukemia (T-LGLL), and mature T cell malignancies.



Inclusion Body Myositis (IBM)
Inclusion body myositis (IBM) is the most prevalent myopathy in adults older than age fifty, with over 50,000 patients estimated in the United States and Europe. This debilitating disease is characterized by progressive weakness and atrophy of muscles of the arms and the legs, as well as muscles involved in swallowing. IBM is chronically progressive and results in severe disability and premature death.
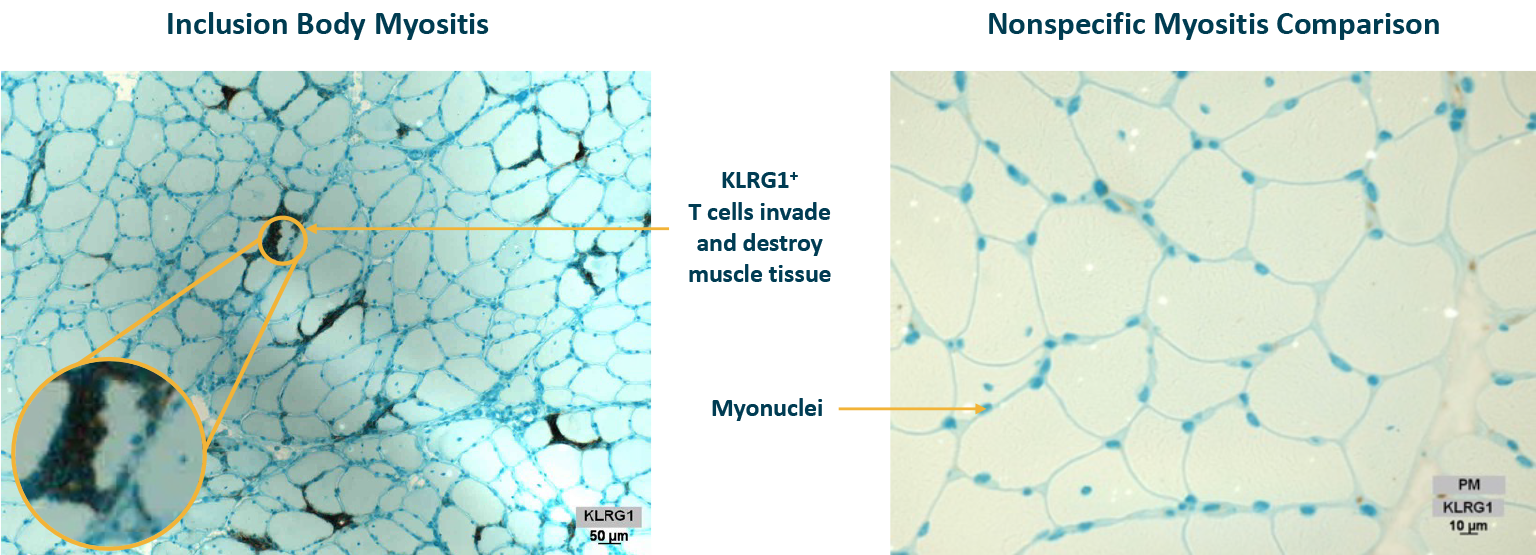
IBM is an autoimmune condition in which highly cytotoxic T cells attack muscle which leads to degeneration of the tissue. Muscle tissue from patients with IBM shows the presence of highly differentiated, KLRG1+ cytotoxic T cells destroying muscle fibers.
There are currently no available therapeutic options for IBM. Non-specific immunosuppressants or corticosteroids have not demonstrated efficacy in IBM and thus, are not widely used.
T Cell Large Granular Lymphocytic Leukemia (T-LGLL)
T cell large granular lymphocytic leukemia (T-LGLL) is an autoimmune disorder characterized by clonally expanded CD3+CD8+ cytotoxic T lymphocytes attacking neutrophils and red blood cell precursors, leading to neutropenia and anemia. Neutropenia causes frequent infections, which are a major cause of premature death in patients with T-LGLL. Anemia results in transfusion-dependence in approximately one third of patients.
Given the lack of approved therapeutic options for T-LGLL, about 50% of patients utilize off-label therapies such as the non-specific immunosuppressant methotrexate. Limited efficacy of current standard of care is reflected in an overall reduced life expectancy for T-LGLL patients.
T and NK Cell Lymphomas
T and NK cell lymphomas are a group of aggressive cancers in the lymph and blood that tend to have poor outcomes for patients. The cancer cells are cytotoxic, well-differentiated and can express KLRG1 as a cell surface marker. Patients with these cancers are treated with powerful cytotoxic agents which have limited sustained efficacy and significant side effects. Abcuro aims to assess the efficacy and safety of Ulviprubart, a targeted depleter of cytotoxic T cells and NK cells that express KLRG1 in patients with this group of severe diseases.


